The Connection Between Intermittent Fasting and Gut Mucosal Integrity
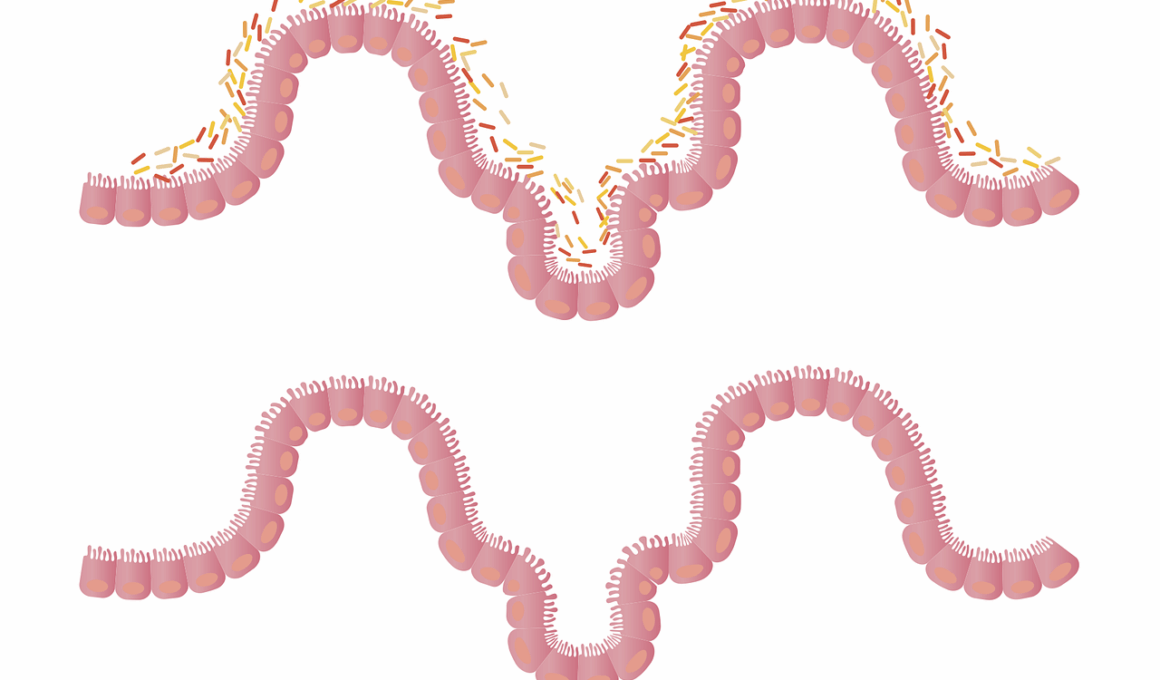
Intermittent fasting (IF) has garnered significant attention for its potential health benefits, particularly concerning gut health. This approach involves cycling between periods of eating and fasting, influencing various biological processes including those related to gut health. One of the most intriguing aspects of IF is its link to gut mucosal integrity, which plays a crucial role in maintaining overall gut health. Research indicates that fasting might help enhance the gut barrier function, reducing intestinal permeability. When the gut barrier is intact, it protects against harmful substances that can lead to inflammation and autoimmune conditions. This is particularly important as the gut microbiota interacts closely with gut mucosal cells. Through the modulation of gut microbiota composition, IF may profoundly impact mucosal integrity. This suggests that individuals practicing IF may not only benefit from weight loss but may also improve their digestive health significantly. Overall, understanding the mechanisms by which intermittent fasting affects gut health can provide valuable insights into implementing dietary strategies for health improvement and disease management.
One of the pivotal roles of gut mucosal integrity is to prevent the translocation of harmful bacteria and toxins into the bloodstream, which can result in systemic inflammation. Periods of fasting may lead to a reset in gut microbiota composition, promoting beneficial bacteria while inhibiting harmful strains. This shift can strengthen the intestinal barrier, enhancing the tight junctions between cells that form the gut lining. In turn, this contributes to better nutrient absorption and overall digestive health. Moreover, studies have shown that intermittent fasting can reduce the occurrence of gastrointestinal disorders, such as IBS or leaky gut syndrome. For individuals facing symptoms related to digestive dysfunction, incorporating intermittent fasting may serve as a therapeutic approach. Additionally, enhancing gut mucosal integrity through fasting can also impact metabolic health positively. As the gut and brain axis plays a role in various physiological functions, the benefits of fasting may extend beyond digestion to improve cognitive functions. This highlights the interconnected nature of gut health with other bodily systems, reinforcing the idea that what we eat and when we eat significantly impacts our overall wellbeing.
Molecular Mechanisms of Gut Health via Fasting
The molecular mechanisms underlying the relationship between intermittent fasting and gut mucosal integrity are complex yet fascinating. Fasting influences various cellular signaling pathways, including autophagy and the production of short-chain fatty acids (SCFAs). Autophagy, a process where cells remove damaged components, is enhanced during fasting, promoting cellular repair. In the gut, this can lead to improved mucosal barrier function, as any damaged cells are efficiently cleared and replaced. Furthermore, during fasting, the gut microbiota produces SCFAs, which have been shown to strengthen the gut barrier function. These SCFAs serve as nutrients for colon cells, promoting their proliferation and health. This indicates that intermittent fasting can facilitate a healthier gut environment. The interaction between the gut microbiome and the immune system is pivotal as well; by enhancing the gut barrier, fasting may help reduce gut inflammation and systemic immune responses. This interplay is fundamental, as a stable gut microbiome contributes to low-grade inflammation, which is associated with chronic diseases. Thus, understanding these molecular mechanisms informs us about how dietary habits can be tailored to optimize gut health.
Moreover, intermittent fasting might lead to the secretion of various gut hormones, including glucagon-like peptide-1 (GLP-1) and peptide YY (PYY). These hormones play significant roles in appetite regulation and promote satiety, which can be beneficial for those aiming to maintain a healthy weight. The relationship between hunger, gut hormones, and mucosal integrity creates a feedback loop where improved gut health may lead to better digestive functions and weight management. Besides, the bioactive compounds present in whole foods consumed during eating windows, such as fiber and polyphenols, can further support gut mucosa health. These compounds directly feed beneficial gut bacteria, promoting a diverse microbiota. The timing of food consumption in intermittent fasting can optimize gut health by allowing the body a break from digestion, reducing the overall workload on the digestive system. This rest period can facilitate healing and repair processes within intestinal tissues, contributing to enhanced mucosal integrity. Therefore, individuals adopting intermittent fasting should focus on nutrient-rich foods during their eating periods to gain maximum benefits for gut health.
Potential Risks and Considerations
While intermittent fasting presents numerous potential benefits for gut mucosal integrity, it is essential to approach this dietary strategy with caution. Not all individuals may respond similarly to fasting. For instance, those with certain health conditions, such as diabetes or eating disorders, may need to avoid or modify fasting practices. Lack of proper guidance and education on how to fast correctly can lead to poor nutritional choices during eating windows, negating the benefits of fasting. Moreover, prolonged fasting without adequate nutrition can contribute to nutritional deficiencies, impacting overall health. It is vital to ensure a balanced intake of macronutrients and micronutrients even during fasting schedules. People should also consult with healthcare providers before starting an intermittent fasting regimen, particularly if they have existing health concerns. Additionally, the psychological impact of stringent fasting rules can lead to stress or anxiety related to food, which can adversely affect gut health. Thus, it is crucial to adopt a flexible approach to intermittent fasting, focusing on fostering healthy eating habits without stress.
Fasting protocols vary in length and frequency, affecting individual responses significantly. Some may find success with a daily 16:8 method, while others may prefer alternate-day fasting or longer fasting periods. The variability in individual metabolism and lifestyle implications requires tailoring fasting methods to enhance its benefits for gut health. For instance, considering one’s age, sex, and level of physical activity plays a vital role in determining the most suitable fasting schedule. Furthermore, monitoring one’s physical and mental responses during fasting can aid in adjusting methods to fit personal needs. Keeping a food diary or using apps to track dietary intake during eating windows can provide valuable insights, helping people focus on gut-nourishing foods rich in prebiotics and probiotics. This approach can promote a healthy gut microbiome, crucial for maintaining mucosal integrity. Lastly, sustaining consistent dietary habits over time promotes lasting benefits. Engaging in education regarding gut health and intermittent fasting can empower individuals to make informed choices, leading to improved overall health and well-being alongside a flourishing gut environment.
Conclusion: Embracing Intermittent Fasting for Gut Health
In conclusion, intermittent fasting shows promise as an effective strategy for enhancing gut mucosal integrity, contributing significantly to overall health. The positive effects of fasting on the gut barrier function, microbial diversity, and hormone secretion demonstrate the deep connection between dietary practices and gut health. While it is vital to emphasize the importance of proper nutrition during eating periods, practicing intermittent fasting with mindfulness can yield impactful results. As more research unfolds, the potential applications of fasting in clinical settings may become clearer, allowing health professionals to recommend this approach as a complementary therapy for various gut-related disorders. Ultimately, embracing intermittent fasting offers a holistic way to improve gut health, promoting wellness across many aspects of life. By understanding the intricate relationship between diet, gut health, and mucosal integrity, individuals can empower themselves to make healthier choices. Encapsulating the benefits of intermittent fasting can lead to enhanced well-being, vitality, and resilience, informing a more proactive approach to dietary choices, ultimately benefiting gut health and proper functioning.
Through this exploration of intermittent fasting and its profound implications, one learns the significance of creating dietary habits that align with personal health goals. Engaging with the principles of intermittent fasting is not merely about restricting food intake; it’s about cultivating a paradigm shift towards longevity and overall health that emphasizes self-care and mindfulness. This transition can foster a deeper understanding of the body’s needs and how best to support gut integrity. With knowledge and informed guidance, individuals can navigate their fasting journey effectively, enhancing their connection to their own health and wellness.